- Home
- Article
Patient Warming’s Preventative Benefits
By: April Smith
Published: 5/25/2021
Maintaining normothermia reduces the risks of negative outcomes, including SSIs.
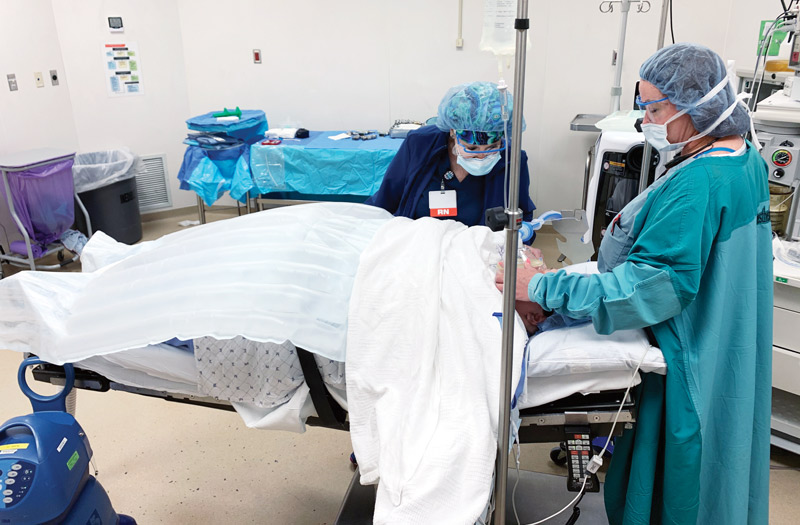
Prewarming is paramount
Although providers might debate the effectiveness of the devices and techniques used to warm patients, there’s no argument about when warming should start. “It should begin the minute patients change into their surgical gowns,” says Melissa Kellam, CRNA, DNAP, a staff anesthetist and clinical coordinator at the Mobile (Ala.) Infirmary.
This thinking on patient warming has evolved in recent years. “Intraoperative warming has historically been embraced as a scientifically proven intervention,” says Michael C. Roberson, PhD, DNAP, CRNA, an independent anesthesia provider in Jackson, Miss., and adjunct faculty member at William Carey University in Hattiesburg, Miss. “However, discussion has ramped up in the last 10 years regarding preoperative warming as an effective way to help maintain normothermia.”
The biggest challenges have been educating physicians and staff on the need for consistent use of prewarming and the collective benefits of starting the process before patients enter the OR, adds Dr. Roberson. Getting buy-in is a lot easier when you can use research to make your case. In fact, Dr. Roberson’s own research supports the need for prewarming patients (osmag.net/rK8HmY).
“Evidence demonstrated that active prewarming helped to attenuate inadvertent perioperative hypothermia,” he says. “Prewarmed patients experienced less post-op nausea and shivering, improved thermal comfort and earlier extubation.”
A prewarming protocol should be the standard for all your surgical patients. However, at the very least, be sure to prewarm patients who are most at-risk for hypothermia. Dr. Kellam points out that patients on certain medications such as tricyclic antidepressants and antipsychotic phenothiazines that exhibit iatrogenic effects on the thyroid can be at higher risk. Patients with thyroid problems of any kind have trouble regulating core body temperatures in the normothermic range. Patients with diabetes are also at high risk.
Leaning into the data is no doubt a good strategy for selling prewarming to surgeons and staff, but don’t forget to tout the satisfaction element, as well. “In too many facilities, the patient is already sedated by the time active warming starts,” says Dr. Kellam. “They wake up warm, but all they remember is being cold before surgery.”
She adds that preoperative warming can prevent patients’ early discomfort and decrease their anxiety, making it easier for staff to prepare them for surgery. It also improves the rate at which anesthetics work. “Patients fall asleep faster when they’re warm,” says Dr. Kellam.
She knows about the benefits of prewarming from both sides of the OR table. “I had to have surgery, and told the staff before they started my IV, ‘Look, I don’t have any veins, so get your best person on it,’” she recalls. “A nurse came in and put a warming blanket on me. My veins perked up and she placed the line on the first try. The experience decreased my anxiety, and I haven’t stopped raving about it since.”
Warm recoveries
Although many facilities have some type of intraoperative warming protocol in place, not enough attention is paid to postoperative warming. “Warm patients wake up quicker because they metabolize anesthetics at an increased rate,” said Dr. Kellam. “If the patient is cold in recovery, it will take longer for them to emerge from anesthesia.”
Whenever Dr. Kellam can’t wake patients up right away in PACU, the first thing she tells the nurses is “Warm them up!” Of course, you should focus on applying warming measures throughout the entire surgical episode, beginning the moment the patient enters the pre-op bay. “The body’s process of waking up from anesthesia involves transferring the anesthetic through blood from the brain to the lungs, where it’s exhaled,” says Dr. Kellam. “That process will go faster when the patient is warm.”
Patient warming can also decrease the length of post-op stays by decreasing pain, thereby reducing the need for sleep-inducing pain medications. “The more shivering the patient does, the more pain they will be in, and their oxygen consumption will increase 200% to 300%,” says Dr. Kellam. “If they’re in more pain, we have to give more pain meds, which will further delay their waking up and being ready for discharge.”
Dr. Roberson shares his own experience with post-op lengths of stay at an outpatient facility that instituted active warming during all orthopedic procedures — regardless of procedural length or type. “Examination of PACU admission temperature data revealed statistically significantly higher core temperatures with resultant shorter PACU stays and therefore expedited discharge from the facility,” says Dr. Roberson. In other words, the universal warming protocol led to faster recoveries and more efficient post-op discharges.
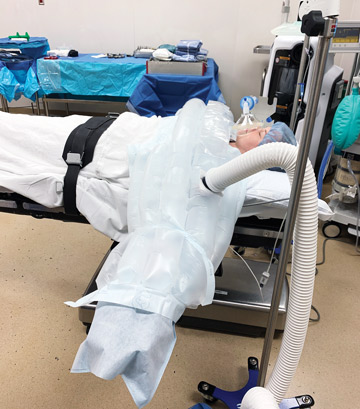
Whether you’re putting together your first patient warming policy or looking for ways to improve an existing one, here are 10 steps your staff should take to make sure patients are properly warmed, according to Melissa Kellam, CRNA, DNAP, a staff anesthetist and clinical coordinator at the Mobile (Ala.) Infirmary:
• If the patient is not pre-warmed, start active warming prior to induction of anesthesia.
• Warm intravenous fluids and blood products to 37°C.
• Warm irrigation fluids used intraoperatively in a thermostatically
controlled cabinet to 38°C to 40°C.
• Document temperature routinely (every five minutes, for example).
• Measure core temperatures whenever possible.
• Induction of anesthesia should
not begin unless the patient’s temperature is 36°C or above.
• Actively warm patients intraoperatively if they’ll be anesthetized for more than 30 minutes or if they’ll be sedated for less than 30 minutes
and are at higher risk of inadvertent perioperative hypothermia.
• The temperature setting on warming devices should be set to maintain a patient temperature of at least 36.5°C.
• Measure and document patients’
temperatures upon admission to PACU and then every 15 minutes thereafter until a normothermic reading is achieved.
• Discharge should not be arranged unless the patient’s temperature is 36°C or above. If the patient’s
temperature is below 36°C, they should be actively warmed until they reach normothermia.
If you’re having trouble determining the right warming device to use at your facility, Dr. Kellam has some simple advice. “If you bring in three different warming systems and the staff says, ‘This is the best one,’ go with that system,” she says. “The method staff members prefer might cost a little more, but it’s well worth the added expense because they’ll be more likely to use it to warm every patient.”
— April Smith
Beyond comfort
A comprehensive patient warming protocol can benefit your facility in many ways, including in cost savings. Research shows that hypothermia add between $2,500 to $7,000 per patient,
says Dr. Roberson.
Plus, public and private insurance companies now tether procedure reimbursements to patient satisfaction, which is a reportable service, and cold patients are generally unsatisfied with the care they receive.
Maintaining normothermia in patients ultimately provides many clinical benefits that are too important to ignore. “Intraoperative hypothermia is not a benign occurrence,” says Dr. Roberson. “Along with increased morbidity, it’s associated with decreased cardiac output, prolongation of muscle relaxants and disruption of clotting factors that slows wound healing, and increased surgical infection rates.” OSM
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)