- Home
- Article
What’s Best for Eye Surgery Sedation?
By: Dara McBride | Contributing Editor
Published: 2/15/2024
Some providers swear by IV anesthesia, while others say a pill to reduce pre-op anxiety is the way to go.
Talk about a strong endorsement: John Berdahl, MD, an ophthalmologist at Vance Thompson Vision in Sioux Falls, S.D., counts his mother and father as patients who have undergone intravenous-free eye surgery.
In fact, Dr. Berdahl has too.
Reduce anxiety, promote relaxation
That’s not to say Dr. Berdahl and his parents relied exclusively on their pain tolerance and strength of character to stay composed during the procedures. Instead, the practitioners at Vance Thompson Vision administer preoperative sublingual methods to reduce anxiety and promote relaxation instead of the traditional IV administration of sedation.
“We’ve had people fly from Florida to have surgery with us simply because they were so needle-phobic,” says Dr. Berdahl. The high-volume eye center at which he works performs everything from cataract and glaucoma surgeries to corneal transplants and anterior segment reconstruction.
Patients with a fear of needles or who have difficulties getting IVs placed in them aren’t the only candidates for alternatives to IV sedation. Dr. Berdahl’s preferred sublingual method provides sedation during cataract surgery without the use of an IV or opioids.
“It’s a very patient-centric approach,” says Dr. Berdahl. “If you’re a patient and don’t need an IV, why would you want one? And if you’re a patient and you don’t need an opioid — you definitely don’t want one.”
In order for the more common IV sedation to effectively reduce preoperative anxiety, healthcare providers must act fast when placing the IV and have an anesthesiologist on hand to monitor the patient. Less involved, sublingual sedation methods are becoming emerging trends at large surgery centers, however, and recent innovations have made such sedatives more convenient and less expensive than past iterations.
Sublingual sedation varies
Providers may opt for long-onset liquid diazepam or brief-onset liquid midazolam placed under the patient’s tongue. The preferred tool at Vance Thompson Vision is an MKO Melt, a sublingual tablet consisting of midazolam, ketamine and ondansetron. Dr. Berdahl’s patients at the Sioux Falls clinic receive the MKO Melt in pre-op about 20 minutes before their surgeries.
Initially, Dr. Berdahl relied on only midazolam over IV sedation — and it worked well — but he and the anesthesia team saw an opportunity to improve. The MKO Melt tablet, which Dr. Berdahl helped innovate, delivers over a five-minute release period. Ensuring patient comfort is of the utmost importance to Dr. Berdahl — and that’s a primary reason why he champions sublingual anesthesia delivery.
“One of the most anxiety-provoking times is before surgery, as people are waiting and ominously getting closer and closer to that moment of surgery. One of the beauties of the melt is that people get sedation before the surgery starts in the preoperative area,” he says. “They’re often lightly snoozing before they go back to the operating room.”
The decision to pursue an IV alternative stemmed from a desire to minimize patient discomfort while also addressing concerns about the prevalence of opioids in traditional sedation methods. Over 4.5 million cataract surgeries take place in the U.S. annually, and patients are treated with fentanyl in about half of them, according to Dr. Berdahl. Given that drug’s addictive properties and the ever-increasing opioid crisis, the objective is to decrease or eliminate opioid use during these procedures.
Cost isn’t a driving factor in the decision to use sublingual sedation, as the tablets are similar in price to that of the IV equipment setup and drugs. Additionally, proponents of sublingual sedation point to the cost savings incurred, as well as the time saved on not needing to administer and monitor IVs. This may lead to improved patient throughput and increase daily volumes. Dr. Berdahl emphasizes that using the MKO Melt does not eliminate the need for an anesthesiologist or CRNA to be present. “One of the questions that I get the most is, ‘Can anesthesia still be involved and still bill for care?’ The answer is, ‘Yes,’” says Dr. Berdahl. “Monitored anesthesia care does not require the use of an IV, but it requires the use of an anesthetic. Midazolam and ketamine are anesthetics and as such are monitored.”
The IV perspective
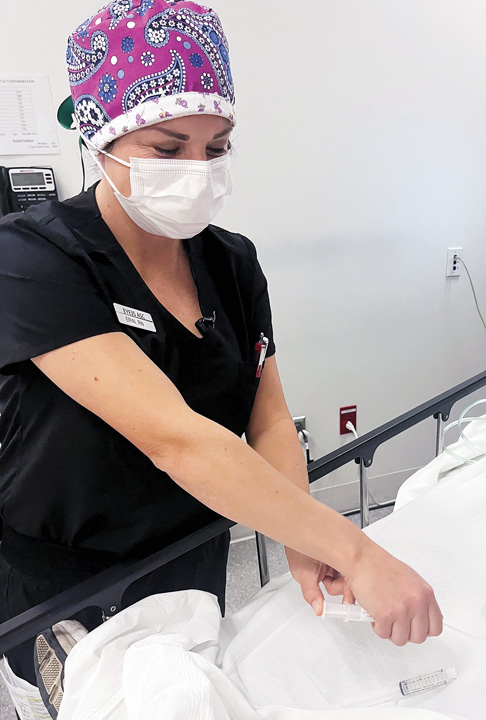
Practitioners at Eye 35 ASC in Schertz, Texas, use IV sedation 100% of the time. Leadership also says they rely on their staff’s bedside manner to help patients relax. The two-room, surgeon-owned ophthalmology clinic performs a variety of procedures, with cataract surgery the most common. It’s understandable that patients arrive feeling anxious and nervous, notes Clinical Director Carson McCafferty, MSN, RN, CNOR, CNAMB, CSRN. “It’s their eyeball! That’s why patients receive a little extra attention when they check in,” she says. “Warm blankets are like little miracles.”
When patients arrive, a nurse collects their vital signs and administers lidocaine drops to numb the eye before setting up an IV to administer sedation — which is typically midazolam followed by fentanyl. Surgeons and CRNAs then work together during the procedure to oversee sedation management.
Moving to nurse-administered sedation represents the most significant shift in patient care at the clinic. In response to a nationwide shortage of anesthesiologists, Eye 35 established its own anesthesia practice staffed by CRNAs. As a smaller and newer clinic, Eye 35 can nimbly provide for its patients, keep pace with its caseload, and stay ahead of staff and medication shortages by doing so.
Ms. McCafferty says the clinic has rarely, if ever, had a patient decline an IV line and that the staff feels confident in their abilities to start them.
“We’re very fast and very efficient. If a patient says they’re uncomfortable or in pain, we’re able to give them medicine on the spot that works in two minutes or less,” she says.
Eye 35’s providers have tried sublingual sedation and understand it works for some facilities, but they ultimately view IV administration as the tried-and-true method with a precise predictability in terms of onset. The combination of midazolam and fentanyl creates “a nice, comfortable environment” for the patient and helps to reduce anxiety, says Ms. McCafferty.
While complications in cataract surgery are rare, there are some cardiac-related ones in patients with previously undiagnosed clinical issues that require hospital transfers, which is a good reason for an IV to have already been established — even when sublingual sedation is used for the actual case. Ms. McCafferty vividly recalls one patient who complained to staff about feeling poorly and registered extremely low blood pressure. That patient, in the clinic for YAG laser surgery, had a blocked carotid artery and was taken to the nearest emergency room.
“We always start a line, even on patients with zero sedation, because you just never know what could happen during the surgery,” she says.
Varying opinions
Efficiency, cost-effectiveness and patient experience are all top of mind when choosing a best practice to follow inside the perioperative suite. In the case of what to choose to help ophthalmology patients relax pre-surgery, the same logic may lead to different conclusions, depending on the clinic and its practitioners. “We’re very much open to change, if it benefits the facility and the patients,” says Ms. McCafferty, emphasizing the importance of communication throughout the practice’s staff and its patients. The clinic often treats patients who have been there before, and its practitioners are able to build relationships and make adjustments to best serve them when they return for subsequent treatments. “We just really want them to leave here and say, ‘That wasn’t bad at all.’ I think for the most part, we do that,” she says.
Meanwhile, Dr. Berdahl remains an advocate for sublingual sedation and uses an additional IV method only when necessary. Clinical trials of the MKO Melt, he says, point to the conclusion that the combined pharmaceutical elements work better together than individually.
“There are a few ways to innovate within medicine,” he says. “One is to provide something that has superior outcomes medically, and this has that. Another way is to make the patient experience better than what traditional medicine provides, and this does that too.” OSM
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)