First, a disclaimer on emerging alternative wound-closure devices: There is nothing superior to the traditional suture in terms of approximating wound edges. On this, plastic surgeon Richard Vagley, MD, FACS, of Spectrum Aesthetics in Coral Gables, Fla., is adamant. Still, Dr. Vagley is bullish on the latest wound closure technologies, 6 of which we profile in this article, that can come pretty close to the precision of a traditional suture in a fraction of the time.
And he isn’t the only one. Asit K. Shah, MD, PhD, an orthopedic surgeon with Englewood (N.J.) Hospital, is also encouraged by recent advances. “Wound closure has never really been improved upon,” says Dr. Shah, “and the bulk of major surgeries have simply been closed by staples.”
But there are plenty of compelling reasons to rethink this status-quo approach to wound closure.
- Patient satisfaction. Dr. Shah recently surveyed his patients on wound closure, and what he found was eye-opening.
“There’s a real fear among patients about having these staples removed,” says Dr. Shah. “With a knee revision, we’re talking about 30, 40 or 50 staples we need to remove.”
In addition to reducing the need for inconvenient follow-up staple-removal appointments, the use of non- or less-invasive adhesive wound closure alternatives can also help with what’s often referred to as the patient’s “halo effect” or overall impression of your facility.
“If a patient sees the surgeon is on the cutting edge and using these staple-free devices, he’s likely to tell his friends and family about your facility,” says Dr. Shah.
- Safety. “I was working side by side with a resident once,” says Dr. Vagley. “I zigged, he zagged, and I wound up with a needle in my finger.” Indeed, accidental pricks that occur with sutures are one of the top causes of injury with sharps among staff. Non-invasive wound closure products remove this sharps safety hazard. Plus, there are patient safety concerns with the more invasive traditional closure devices like staples. “With staples, you’re leaving little holes in the body,” says Dr. Shah. “That’s a possible source of infection. It hasn’t been clinically proven, but it’s always a concern for surgeons.”
- Time savings. This is a biggie, especially for facilities that might balk initially at the increased cost of alternative wound closure products. Sutures and staples are relatively inexpensive when compared to alternatives. “You may be paying $20 for staples versus, maybe, $80 for some type of alternative closure device,” says Dr. Shah. “That shouldn’t be a prohibitive cost — especially if you’re looking at the big picture.” For staples, that big picture involves all the time you’ll save not having to remove staples from patients after surgery. Staple removal becomes like a minor procedure that keeps surgeons from seeing other patients, notes Dr. Shah.
- Ease of use. Many of the closure products available are so simple and intuitive to use, surgeons can delegate the closure to a surgical assistant, something that becomes invaluable in high-volume facilities. “If you’re operating in 2 rooms at a busy facility, and you can delegate the closure to an assistant,” says Dr. Vagley, “there’s potential to complete more cases per day.”
.svg?sfvrsn=be606e78_3)

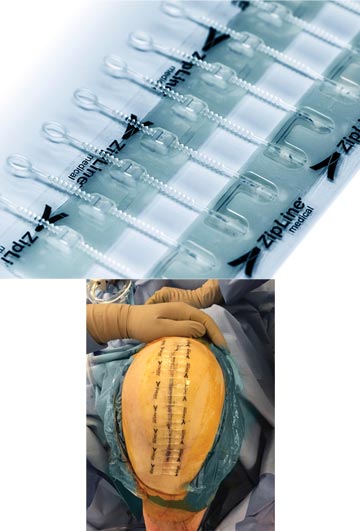
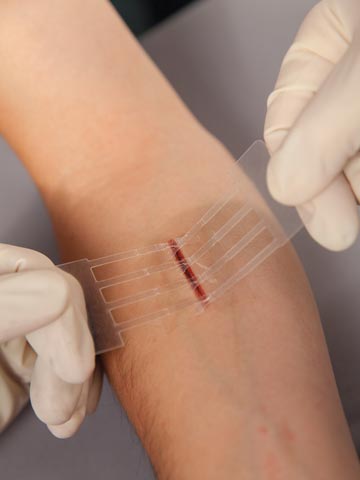


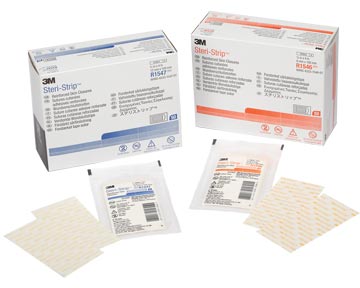

.svg?sfvrsn=56b2f850_5)