More than ever, older patients are doing everything within their power to stay active longer. For many with osteoporotic pressure injuries, multiple treatments often don't give them the relief they deserve from pain and discomfort. A balloon kyphoplasty often succeeds when more conservative options fail and gives once frustrated patients the freedom to enjoy their retirements in the ways they'd dreamed they'd be.
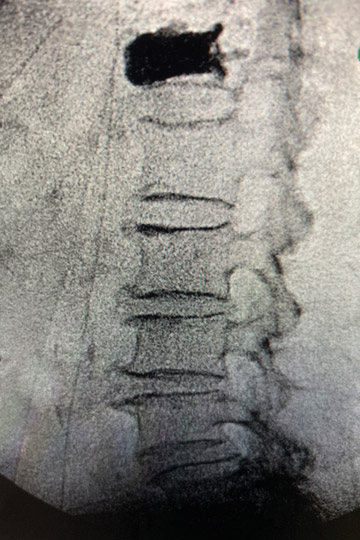
Balloon kyphoplasty is used primarily for patients with osteoporotic compression fractures that have failed conservative management techniques. They've tried immobilization, braces and physical therapy, as well as anti-inflammatories and pain medication. For unknown reasons, those strategies have proved unsuccessful and their discomfort continues. The candidate for balloon kyphoplasty is someone with significant pain that correlates to the level of the fracture as shown in the MRI findings.
The procedure was introduced more than 20 years ago as an alternative to vertebroplasty. Today, the two interventions are the most common forms of surgery to heal vertebral compression fractures. Vertebroplasty is simply the injection of polymethyl methacrylate (PMMA), commonly known as bone cement even though it's actually an acrylic, into the vertebral body.
The addition of the balloon brought multiple advantages. In many cases the balloon procedure can restore some of the vertebrae height that has been lost. Doing so is important, because if the height isn't restored, added pressure is applied to the levels above and below the fractured vertebrae, making them more susceptible to breaking. The balloon also creates a cavity into which the PMMA is injected. The beauty of creating the cavity is you can use PMMA that has a higher viscosity. The low-viscosity PMMA used during vertebroplasty can extravasate beyond the vertebral body. The higher-viscosity PMMA that can be used with balloon kyphoplasty has the consistency of toothpaste, making it easier for surgeons to achieve their goal of containing as much of the PMMA as possible within the vertebral body. The balloon makes the procedure safer and more predictable than a simple vertebroplasty.
Promising instrumentation systems have recently hit the market that allow for increased accuracy as to where within the vertebral body surgeons can place the balloon. In some cases, they like to place it at the superior plate, while other times they'd prefer to place it in the interior or central part of the vertebral body. The more options surgeons have the better, because outcomes improve with the increased ability to steer the placement of the balloon.
The technology of the balloons themselves has also progressed quite nicely. They're now much less likely to burst, and surgeons are able to inflate them to much higher pounds per square inch. We've gone from having to make multiple instrument exchanges to using an all-in-one device. There have also been advances in the tip of the trocar, which is now directional and beveled.
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)