Last year marked the 20th anniversary of the Needlestick Safety and Prevention Act, landmark legislation that was intended to eliminate the sharps injuries that continue to occur today. In fact, OSHA estimates 5.6 million healthcare workers and related occupations are at risk of occupational exposure to bloodborne pathogens, including HIV, hepatitis B and hepatitis C.
Something needs to change. Safe sharps handling practices are important, but the best way to protect your surgeons and staff from sticks and cuts is to eliminate the devices that cause them.
• Identify the issues. Janice Kilby, RN, MAN, MN, CNOR, a practice consultant at Kaiser Permanente Mid-Atlantic States (KPMAS), worked with colleagues to establish a multidisciplinary sharps safety council, which develops and maintains comprehensive programs aimed at eliminating occupational exposures to bloodborne pathogens throughout the health system. “We track sharps injury rates and analyze the nature of each injury, including the device, profession and job function involved,” says Ms. Kilby.
She suggests maintaining a sharps injury log, which OSHA says should include the type and brand of devices involved in exposures, the department or work area where exposures occurred and explanations of how the incidents happened — while maintaining the confidentiality of the staff members involved. Use the log to conduct quarterly reviews of your facility’s sharps injuries to determine if they were related to product design, device failure, clinical factors such as sudden patient movement or the activity being performed. Then design and implement sharps safety education programs and campaigns based on problem areas or injury types. By analyzing the trends on a regular basis, you’ll identify who’s most at risk for injuries and why they occurred — the information you’ll need to implement safer practices.
“We found that about 30% of sharps injuries involve surgeons, because they perform delicate procedures in the surgical field,” says Ms. Kilby. “We also discovered that syringes are involved in 40% of injuries, because of the intricacies involved in giving an injection, activating the syringe’s safety mechanism and properly disposing of the used needle.”
Deborah L. Spratt, MPA, BSN, RN, CNOR, CHL, a perioperative consultant at St. James Hospital/University of Rochester (N.Y.) Medicine, hopes sharps safety is addressed at all facilities with yearly education, regardless of the number of exposures they record. “Our experience showed that it was only when an organization identified a significant number of injuries that they created a group to actually work on solutions,” she says.
Ms. Spratt believes facility leaders should proactively promote sharps safety and the use of safety-engineered devices instead of waiting for injury rates to climb before taking action.
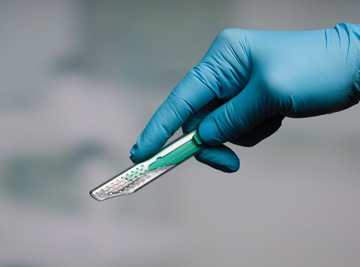
• Require exceptions. The Needlestick Safety and Prevention Act requires your facility to trial safety-engineered devices — such as sharps disposal containers, self-sheathing needles and safety scalpels — on an annual basis in order to identify and implement safe options. Requiring your staff and surgeons to opt out of using sharps safety devices helps to increase compliance with this element of the legislation.
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)