You must protect your staff from harm so they can properly care for their patients. Prioritizing their health and well-being requires a mix of consistent and effective education and training, a heightened degree
of mindfulness, solid evidence-based protocols, and the use of helpful adjunct technologies and products. See how you do in answering the following questions to determine if you need to refocus your efforts on protecting your hardworking
providers.
1. According to the International Safety Center and U.S. EPINet's 2019 Sharps Injury Data Report for Needlestick and Sharp Object Injuries, what percentage of injuries were caused by devices that featured shielded, recessed, retractable, or blunted needles or blades?
- a. 13%
- b. 38%
- c. 52%
- d. 62%
- Reveal
Answer: c
Yes, about half of sharps injuries are inflicted by devices that are designed to be safer for staff to use. It shouldn't be surprising then, that in 71.6% of those instances the safety mechanism was not
activated when the injury occurred. "What happens, particularly in the OR, is that people are so hyper-focused on patient safety that they forget to consider their own safety," says Barbara DiTullio, DNP, RN, MA, CNOR,
NEA-BC, senior clinical operations liaison of perioperative services at Beth Israel Deaconess Medical Center in Boston. Conversely, she says some surgeons simply refuse to use safety devices for various clinical reasons
and matters of personal preference. The take-home point here is that safety-engineered devices alone will not eliminate the risks of sharps injuries at your facility; other interventions, including double gloving, more
mindful communication and self-awareness among staff, reducing distractions in the OR and consistent staff education must be considered as part of a sharps safety protocol.
Close
2. What is the first thing OR personnel should do if a surgical fire erupts on a patient?
- a. Remove the burning materials from the patient
- b. Call for help within the building
- c. Alert employees outside the OR to the danger
- d. Stop the flow of anesthetic gases to the patient
- Reveal
Answer: d
Gases feed fires, so removing the oxidizer sources by immediately disconnecting the breathing circuit will cause the fire to go out or at least become less intense, according to Chris Schabowsky,
PhD, CCE, director of accident and forensic investigation services at ECRI, an independent nonprofit organization focused on improving healthcare safety, quality and cost-effectiveness based in Plymouth Meeting, Pa.
"Disconnection of the breathing circuit can also facilitate moving the patient rapidly, such as to another OR," he says. "This is particularly important for airway fires in which the anesthetic gases are being directly
applied to burning materials inside the patient." ECRI, which estimates that approximately 100 surgical fires occur each year in U.S. ORs, teamed up with the Anesthesia Patient Safety Foundation to produce a free
downloadable poster that details steps staff should take not only when a fire is on a patient, but also in case of an airway or breathing
circuit fire. To prevent fires from happening in the first place, Dr. Schabowsky recommends performing thorough preoperative fire risk assessments during time outs, discussing fire risks involved with the procedure
as well as what each surgical team member should do to reduce the risks. He adds that teams should make sure potential ignition sources are used appropriately and placed in standby when not in active use, and use the
minimum amount of oxygen required to adequately support a patient throughout a procedure.
Close
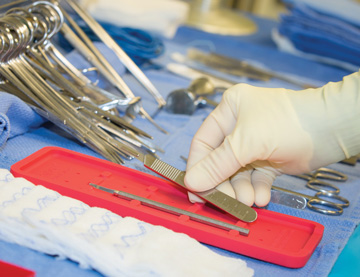
SHARP ENGAGEMENT OR staff and surgeons must practice mindfulness and effective communication while passing sharp objects during surgeries. | Pamela Bevelhymer, RN, BSN, CNOR
3. According to the CDC, which step should be done first when donning a mask?
- a. fit the flexible band to the bridge of the nose
- b. fit snug to face and below the chin
- c. secure ties or elastic bands at the middle of the head or neck
- d. check the fit
- Reveal
Answer: c
Even if you properly don masks every time as described in the correct answer, it’s always helpful to renew your focus on those steps. Even when providers have the best intentions of properly
donning and doffing, circumstances in the moment can be distracting. Like any routine in life, bad habits can form over time. "It's baffling when staff and physicians don't always comply with something as straightforward
as surgical attire policies," says Chris Hunt, MBA, MS, BSN, RN, CSSM, a Seattle-based perioperative nurse executive and consultant. He says there are many reasons this can occur: decades of individual practice, tradition,
insufficient — and sometimes conflicting — research backing the importance of properly wearing PPE and professional disagreement. As the nation continues to navigate the COVID era, the virus' rapid spread
in some areas can be a source of anxiety and frustration for some providers when donning and doffing PPE; in areas where it's currently under control, a false sense of security can set in for some providers. While it’s
always important to refresh and enforce proper PPE protocols at your facility, it's never been more important than right
Close
4. How many hazardous chemicals and carcinogenic and mutagenic cells can be found in surgical smoke?
- a. 16
- b. 30
- c. 78
- d. 150
- Reveal
Answer: d
Perhaps the most well-known statistic associated with surgical smoke is that a day spent in an OR during smoke-generating procedure is the equivalent of smoking 30 unfiltered cigarettes, but this
one is no less shocking. Jennifer Pennock, senior manager of government affairs for the Association of periOperative Registered Nurses (AORN) and a key driver in efforts to mandate usage of smoke evacuation systems
in ORs in all 50 states, lists the alarming aspects of the smoke-producing environments in which surgeons, staff and patients regularly find themselves. "Surgical smoke contains toxic gases and vapors, such as benzene,
hydrogen cyanide, formaldehyde, bioaerosols, dead and live cellular material, blood fragments and viruses," she says. "In addition to causing respiratory illness, asthma and allergy-like symptoms, surgical smoke contains
live viruses such as human papillomavirus, and can cause cancer cells to metastasize in the incision site of patients having cancer removal surgery." If you’re not yet mandating the use of smoke evacuators at
your facility, take advantage of the resources available through AORN's Go Clear program.
Close
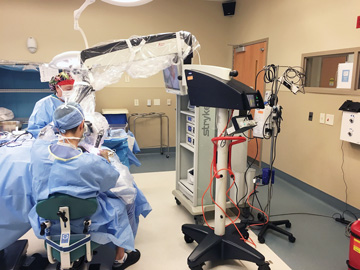
PERFECT PLACEMENT Booms, equipment cabinets and cable management systems can keep thickets of cabling off the floor and out of high-traffic areas in the OR. | Piedmont Outpatient Surgery Center
5. In a massive quality improvement study conducted from 2011 to 2018 published in JAMA Open Network, more than 2.9 million simulated phishing emails were sent to employees at six hospitals. How many of those emails were clicked on by healthcare employees?
- a. 1 in 134
- b. 1 in 32
- c. 1 in 7
- d. 1 in 4
- Reveal
Answer: c
Phishing is a social engineering tactic used by hackers in which they send fraudulent emails designed to trick employees into revealing sensitive information or to deploy ransomware on the employee's
machine in order to access the company network. The plain fact is that successful phishing attacks can cause so much financial and operational havoc that your surgical facility's entire business could be in jeopardy.
"Email phishing is a major attack vector against hospital employees," say the authors of the study, and there's no doubt that ASCs, which often don't possess the cybersecurity infrastructure of hospitals and large health
systems, are in cybercriminals' sights as well. To prevent cyberattacks, employ a three-pronged strategy recommended by Northwell Health Chief Information Security Officer Kathy Hughes: Educate your staff — starting
with yourself, if need be — on how to recognize and always be mindful of potential phishing emails; employ security technologies such as anti-malware and encryption systems; and keep those security technologies
airtight by always installing the latest updates as soon as possible.
Close
6. In an Outpatient Surgery Magazine survey of 379 facility leaders, what percentage said one of their staff members or surgeons had sustained an injury from slipping or falling in the OR?
- a. 14%
- b. 29%
- c. 51%
- c. 60%
- Reveal
Answer: d
These anecdotal results indicate that slipping and tripping hazards remain an issue. An even more alarming finding that emerged from the survey: 25% of the injuries reported were serious. If slips,
trips and falls are a problem at your facility, it's worth a close look at the layout of your ORs, as well as how your staff and surgeons move around the room during surgeries. The problem areas will likely become
obvious. Anjali Joseph, PhD, EDAC, director of the Center for Health Facilities Design and Training at Clemson (S.C.) University, suggests consolidating equipment in ORs by eliminating carts and towers in favor
of floor- or ceiling-mounted booms that also keep floors free of cables and wires. She also suggests organizing ORs into dedicated work zones to minimize steps and limit movement during cases, and providing circulating
nurses with mobile workstations to limit their walking around the sterile field during surgery while simultaneously allowing them to easily move aside when needed to ensure high-traffic areas remain clear. Other
solutions can include installing extra outlets to keep cabling runs to a minimum, leveraging cable management systems that gather wires together or hide them from view, and using absorbent mats and fluid management
systems to keep floors dry.
Close

BAD AIR Once they learn how many chemicals, carcinogens, biological material and viruses can be found in surgical smoke, it’s difficult for many safety-focused providers to forget.
7. According to AORN guidelines for radiation safety, how often should radiation protective garments be cleaned and disinfected if they are only worn by one person?
- a. three times daily
- b. once daily
- c. once weekly
- d. monthly or when soiled
- Reveal
Answer: b
AORN guidelines state that radiation protective garments such as thyroid shields, vests and skirts should be cleaned and disinfected daily if worn by one person, and between uses if worn by more
than one person. The organization also notes that those who clean and disinfect these garments and devices should employ the exact cleaning methods stated in the manufacturer’s instructions for use. According
to Angela Ellis, MSN, RN, CNOR, a perioperative clinical specialist at H. Lee Moffitt Cancer Center in Tampa who presented a poster on the subject at the 2019 AORN Surgical Conference and Expo, these guidelines
are far from widely implemented. "People at the conference were floored by it," she says. "We repeatedly heard, 'We don’t have a process in place for this.' It's just something that's overlooked."
Ms.
Ellis' and her colleagues developed this protocol if you’re faced with a similar situation at your facility: Establish a cleanliness baseline using microbial wipes and/or fluorescent markers to test compliance;
find out who is currently accountable for cleaning the devices and ask them about their practices and frequency of cleaning to get a sense of how large their knowledge deficits might be; provide staff education
including hands-on demonstrations on proper techniques; maintain compliance over time through visual observations and secret use of fluorescent markers; and ensure that garments are stored properly so they don't
develop breaches of integrity.
Close
8. According to OSHA, workers in healthcare settings are _____ times more likely to be victimized by workplace violence than workers in private industry.
- a. 0.5
- b. 1.5
- c. 3
- d. 4
- Reveal
Answer: d
OHSA also reports that approximately 75% of the nearly 25,000 workplace assaults reported annually occurred in healthcare and social service settings. In a Sentinel Event Alert published in 2018,
The Joint Commission encourages healthcare organizations to address this growing problem by implementing these several suggested actions. Start by clearly define workplace violence and put systems into place across
the organization that enable staff to report workplace violence instances, including verbal abuse. It's also important to capture, track and trend reports of workplace violence, including verbal abuse and attempted
assaults. Provide appropriate follow-up and support to victims, witnesses and others affected by workplace violence. Review each case of workplace violence to determine contributing factors, and analyze data related
to workplace violence to determine priority situations for intervention. Develop quality improvement initiatives to reduce incidents of workplace violence and train all staff in de-escalation techniques, self-defense
and proper response to emergency codes. Finally, constantly evaluate workplace violence reduction protocols to determine the effectiveness of the initiatives. OSM
Close



.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)