When Stamford Health (Conn.) discovered a lack of standardization in its skin antisepsis protocols, the OR leaders at the facility knew they had act. After all, inconsistency is the enemy of an effective prepping process.
Although Stamford did have a policy in place for skin antisepsis, pre-op practices needed to be updated and improved upon. "There was no way of identifying if patients were in compliance with our requirements because there was no uniform policy for documenting it, and no way to validate the process if it was completed," says Racquel Swaby, BSN, BN, CPAN, nurse manager of perioperative services at Stamford Health. "We had long-established pre-op prepping protocols for cardiac patients where every patient would come in, have their hair clipped around the surgical site and receive CHG wipes."
But the inconsistency involved in applying the pre-op protocols to other patients was a major problem. The health system wanted to follow AORN recommendations and ensure that every patient received some form of skin antisepsis before entering the OR, says Ms. Swaby.
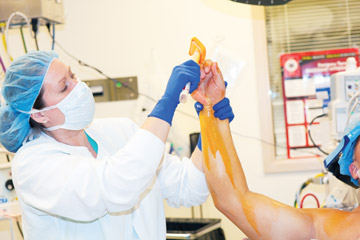
With the gap in its skin prep protocols uncovered, Stamford got to work and fixed the problem. First, it changed its policy and required pre-op assessments to include confirmation that all patients prepped their skin at home with either antibacterial soap or 2% chlorhexidine gluconate (CHG) wipes. (The wipes are required for all total joint, spine and cardio patients). If nurses discovered that a patient didn't comply with the antisepsis policy, the prepping process was completed in the pre-op area.
The facility also ramped up its patient education efforts. "We wanted to make sure that every patient was given clear information, based on their procedures, about what they needed to do for skin antisepsis," says Ms. Swaby.
For instance, information on whether the surgical procedure warranted CHG cleansing at home on the days leading up to surgery was included in information packets given to patients when their cases were scheduled. Finally, Stamford developed a pre-op skin prep assessment tool nurses use to document what they discovered in the pre-op phase. "We worked with our informatics partners to develop a tool that nurses could use to enter information directly into our EMR," says Ms. Swaby.
The major benefit of the assessment tool is being able to track whether the surgical team is compliant with best prepping practices and identify staff members who may need extra education on ensuring patients' skin is properly treated before surgery. "It's a way for us to look back at individual charts and say, 'OK, was this patient assessed for pre-op prep, yes or no?'" explains Ms. Swaby.
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)