- Home
- Special Editions
- Article
Navigating Cataract Reimbursement Challenges: A Guide for ASCs and Surgeons
By: Blake K. Williamson MD, MPH, MS, and Kirk A. Mack, COMT, COE, CPC, CPMA
Published: 2/14/2024
How to maximize your revenue and boost your efficiency.
As the cataract reimbursement scene keeps changing, surgeons and facility leaders must feel like they’re on a roller coaster they never agreed to ride in the first place. Most physicians didn’t sign up for the business side of medicine, but in today’s healthcare environment it can’t be avoided.
The current financial landscape — especially as it pertains to cataract reimbursement — tells a tale of contrasting trajectories for surgeons and outpatient facilities. While Medicare surgeon fees have seen a downward trend over the last several years, facility fees for ASCs and HOPDs have actually risen, thanks to the Hospital Market Basket, a measure used in healthcare economics to track and analyze changes in the cost of goods and services provided by hospitals.
Budget neutrality
Why is this gap in reimbursement happening? This disparity is rooted in the government’s pursuit of budget neutrality — the belief that spending on Medicare should have no budgetary impact — which is forcing a delicate balancing act between reducing payments to facilities or to surgeons. In other words, any additional costs incurred due to changes in one aspect of the program should be offset by savings or reductions in another. As surgeons have become more efficient and spend less time in each case, payors are trying to adjust the payments for surgeon fees. The right adjustment is especially important to the government’s bottom line, as cataract surgery is one of the biggest costs to Medicare.
Increased scrutiny through audits and the introduction of costlier drugs adds even greater complexity to the reimbursement equation. The discrepancy in reimbursement trends between ASCs and surgeons underscores the need for strategic responses to ensure financial sustainability.
Countering reimbursement challenges
Facing the current reimbursement challenges just described, ASCs and surgeons must work together on strategic approaches to maintaining financial viability. While the specifics will differ from center to center, the approach should include:
• Operational efficiency optimization. ASCs should conduct a thorough review of their operations, addressing both staffing and cost structures. Start by taking a close look at your staffing to make sure you’re not running too heavy or too lean with your numbers. You also want to review your costs for cataract packs and goods. Many vendors offer bundling, which can save you money simply by using the same brand for multiple instruments or pieces of equipment.
We’re also seeing a push to stop penalizing surgeons who perform bilateral cataract surgery.
The goal is to be as efficient as possible with the cataract procedure. At our eye center, that efficiency comes from an extremely structured setup with two adjacent ORs running simultaneously. With this setup, the surgeon can quickly move back and forth from case to case to maximize efficiency. We perform 30 to 35 cases per morning, thanks in large part to the efficiency of this setup.
Staff also regularly review our efficiency to make sure we’re maximizing our time — and making adjustments when necessary. For instance, when we noticed our surgeons’ “dead time” was creeping up from 50 minutes to 80 minutes a day, we talked with our staff about ways to identify areas of inefficiency and address them accordingly. We understand there can’t always be zero minutes of dead time — sometimes patients have a problem dilating or something is running behind — but ideally, surgeons want to maximize their throughput as much as possible.
Finally, when it comes to efficiency, don’t shy away from consultants. Consider reaching out to companies with experts in the outpatient space that can audit your center, identify inefficiencies you may have missed and offer helpful solutions.
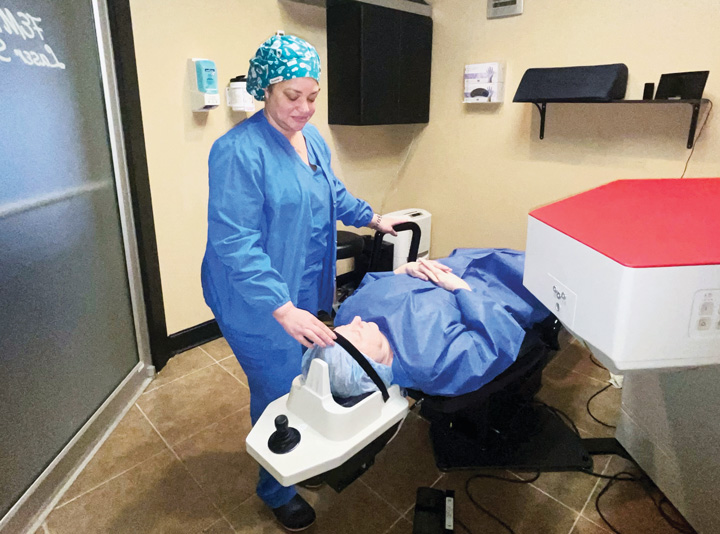
• Femtosecond laser utilization. The efficient use of femtosecond lasers has emerged as a key strategy for surgeons. Delegating laser tasks to physician assistants (PAs) or retired surgeons can significantly increase throughput, enabling surgeons to handle more cases in less time. We have a PA who handles our femto laser for cases.
While some ASCs keep the femto in the OR and designate a single surgeon to perform both steps, we’ve found having a separate suite with a different shooter has saved us tons of time. Patients are walked to the femto room to receive the laser treatment before moving to a nearby OR to continue the surgery. If our surgeon had to run the femto, we would easily add several minutes to each case.
• Diversify beyond standard cataract surgery. If you haven’t done so already, your facility should absolutely look to diversify your services by incorporating premium offerings into your procedures. The big one is premium intraocular lenses (IOLs). These lenses — and the associated work that isn’t covered by insurance — have the potential to generate additional revenue and provide patients with a wonderful experience. Unlike standard IOLs, patients opting for premium IOLs typically don’t need reading glasses.
Compared to a procedure that would be fully covered, premium IOLs have a cash-pay component, which usually comes out to a few thousand dollars. Whether it’s astigmatism or a presbyopia correction, bumping up your adoption rate of these lenses can help your bottom line and leave your patients happier, too. In fact, our center provides Lasik touch-up or lens exchanges for these patients if they’re unhappy. While adding this option to your practice could mean extra chair time, the reality is that 99% of patients are pleased with their surgery and don’t need those extra touches.
Finally, exploring newer technologies like microinvasive glaucoma surgery (MIGS) procedures presents an opportunity for growth, benefiting both your business and your patient outcomes. Performing MIGS procedures can help your facility generate additional revenue while also giving patients much-needed relief from using multiple drops per day. It’s a win all around.
Future outlook for ASCs
The future of cataract reimbursement poses both challenges and opportunities. Although there’s a continued race to the bottom in terms of surgeon reimbursement, there is movement that’s pushing the procedure into innovative territory. This push includes the potential inclusion of office-based surgeries in Medicare reimbursement, which would be a huge change for the industry.
We’re also seeing a push to stop penalizing surgeons who perform bilateral cataract surgery. Overcoming this hurdle could ease the process for patients and potentially lead to increased fees, benefiting both surgeons and ASCs. Some critics cite the fear of complications like bilateral simultaneous endophthalmitis as a reason for slow adoption. However, when the surgeon performs the bilateral procedure following all necessary precautions, the real chance of these feared complications occurring is pretty close to zero.
Currently, surgeon and ASC reimbursement for the second eye is cut in half when facilities do both eyes in the same session/same date of service. But maybe if CMS bumped that second eye’s reimbursement rate for both the surgeon and ASC up to north of 80%, more surgeons would consider offering bilateral cataract surgery to their patients. This not only would increase patient satisfaction — as it means fewer appointments, issues and overall headaches when you can do both eyes in the same day — but it also would allow surgeons to perform more cases.
In the face of evolving cataract reimbursement challenges, facilities and surgeons must adopt proactive and collaborative strategies. Optimizing operational efficiency, embracing diversification and preparing for future changes are critical steps in ensuring the continued success of ASCs in this dynamic healthcare landscape. OSM
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)