From biological indicators to sterilization containers, here’s a breakdown of the latest weapons you can add to your bug-busting arsenal as part of a bundled approach for reducing the risk of surgical site infections (SSIs).
- Home
- The Magazine
- Article
5 Innovations in Infection Control
By: Dan O'Connor
Published: 1/15/2019
The latest products and practices to help you bust those bugs.

1 Rapid readout technology. There is now a 30-minute biological indicator (BI) for all Sterrad (hydrogen peroxide gas plasma) sterilizers. Until now, the only approved BI couldn’t be read for 24 hours. However, with the Sterrad Velocity, it is now feasible to hold the sterilized load until the BI is read, says Luci Perri, RN, BSN, MSN, MPH, CIC, FAPIC, founder and president of Infection Control Results, based in North Carolina. The BI is compatible with all features of the Sterrad sterilizer, including a touchscreen reader with results that can be sent directly to a computer, she adds.

2 Nasal decolonization. The practice of nasal decolonization using a topical antibiotic in specific patient populations has been largely replaced with non-antibiotic nasal antiseptics that to date have not shown any antimicrobial resistance, says Phenelle Segal, RN, CIC, FAPIC, president of Infection Control Consulting Services.
“They’re fast acting, have a persistence that lasts for several hours before having to reapply, and the alcohol-based product has a pleasant citrus aroma,” adds Ms. Segal.
Nasal bacteria are a primary component in the spread of infection. Nasal antiseptics have obviated the need to apply the antibiotic product for 5 to 10 days, which often results in non-compliance and antimicrobial resistance. In addition, nasal antiseptic decolonization is replacing the need to “screen and isolate” patients colonized with multi-drug resistant Staphylococcus aureus such as MRSA, which saves money, time and other resources.
The use of nasal antiseptics before surgery has become a key strategy in the prevention of SSIs as part of the SSI bundle. The SSI bundle includes the use of antiseptic bathing products containing chlorhexidine gluconate.
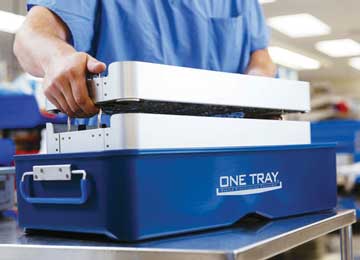
3 Rapid sterilization. Now you can process your vendor trays in a fraction of the time it takes with sterilization wraps and other rigid containers. One Tray, a sealed sterilization container, can terminally sterilize surgical instruments, implants and drills in a prevacuum cycle in less than 20 minutes, rather than 2 hours.
“With the growing demand for faster turnover of surgical procedures, particularly in high-volume situations, reprocessing of medical devices in a timely fashion has been an ongoing challenge,” notes Ms. Segal.
One Tray is ideally suited for high-turnover loaner sets. The containers provide for the safe storage, transport and ensured delivery of the enclosed devices in a sealed container with tamper-evident security and load record documentation. It eliminates the waste associated with the wrapping of surgical instrumentation and orthopedic loaner sets.

4 Transportation labels. Are you transporting clean instruments to the OR and then using the same system to transport dirty instruments to your sterile processing department? One frequently encountered problem when using the same bin or cart for both clean and dirty instrument transport is the lack of a biohazard symbol, which places the facility in violation of OSHA’s Bloodborne Pathogen Standard, says Ms. Perri.
One innovative solution is the Transportation Identification Tag, Healthmark’s 2-part labeling system. The top layer is the “clean” label while the bottom label contains the biohazard symbol labeled “dirty.” When dirty, you simply remove the “clean” label by pulling from left to right. The adhesive backing doesn’t leave residue, so this system won’t increase cart or bin cleaning time, notes Ms. Perri.
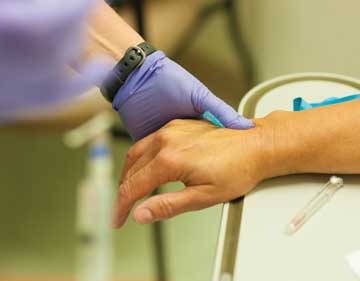
5 Prevent infection during anesthetization. The Society for Healthcare Epidemiology of America (SHEA) recently published expert guidance for infection control in anesthesia workspaces (osmag.net/ BFkwR2). This guidance provides practical solutions consistent with infection control best practices. It clarifies when hand hygiene should be performed during anesthesia care, suggests wearable alcohol hand sanitizer to increase access for anesthesia personnel and recommends double-gloving during airway management, says Ms. Perri.
“Double-gloving lets the provider remove the outer gloves quickly after airway manipulation, which reduces the potential to contaminate the environment and anesthesia work area,” says Ms. Perri.
Additionally, the guidance discusses such important topics as injection safety, length of time between spiking and using IV solutions, required personal protective equipment (PPE) for central line insertion and cleaning and disinfecting high-touch anesthesia surfaces between cases to avoid “drawer-to-arm phenomenon.”
Put yourself at your anesthesia workstation, about to inject a patient with a local anesthetic as she awaits a routine surgery. You reach first to your station for a swab, then back to the patient. Then you go back to your station for a syringe, reach for the vial in one of your drawers, fill the syringe and then back to the patient to inject them with the anesthetic. Every time one of your anesthesia providers make one of those pre-injection steps, every time you touch a drawer on your hard-to-clean workstation for a vial or a syringe or a swab, you’re increasing the risk of contamination. OSM

Skull cap or bouffant? Whichever you prefer, says the 2019 AORN Guideline for Surgical Attire, noting that multiple studies show no significant difference in SSI rates for skullcaps compared to bouffant caps. “No recommendation can be made for the type of head or beard covers worn in the semi-restricted and restricted areas,” reads the guideline (osmag.net/Zyx7KJ), available for public comment until Feb. 22.
Many accused AORN of trying to ban traditional skull caps and force OR personnel to wear bouffant caps a couple years ago. Not true. AORN’s attire guideline stated that perioperative personnel should cover their head and ears in the OR, but it didn’t specify the type or style of head covering that should be worn.
Yet some misconstrued “cover scalp, hair and beards” with “but not with a skull cap.” The confusion likely stemmed from AORN’s rebuttal to the American College of Surgeons’s (ACS) 2016 endorsement of skull caps, hailing them as “symbolic of the surgical profession” and saying that it was acceptable for “only a limited amount of hair” on the nape of the neck and “modest sideburns” to be left uncovered by surgeons wearing skull caps.
AORN challenged the ACS’s tacit approval of exposing the nape of the neck and sideburns. AORN also took umbrage with “wearing a particular head covering based on its symbolism,” saying nationwide practice recommendations should be evidence-based. Many mistook that as an indictment against skull caps.
“Several types of evidence exist,” AORN wrote, “that support recommendations that perioperative personnel cover their head and ears in the OR.”
That much hasn’t changed, nor has the answer to the skullcap-or-bouffant question. The type of hair covering is still each perioperative team member’s choice, says AORN, just as it’s always been. So long as you cover scalp, hair and beards when entering the semi-restricted and restricted areas.
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)