Soon after a total joint or a colon resection patient settles into his pre-op room at Mercy Health St. Elizabeth Boardman (Ohio) Hospital, he's greeted by a nurse holding a box of tissues in one hand and a package of antiseptic nasal swabs in the other.
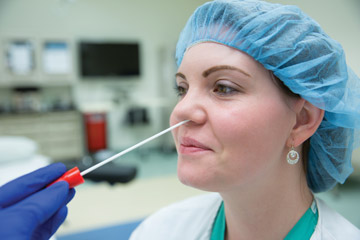
She offers him a tissue and asks him to blow his nose. Then the nurse tilts the patient's head back, opens a 4-pack of povidone iodine swabs and swirls the inner and anterior rim of each nostril for about 15 seconds apiece, and then repeats the process. If preferred, the patient can swab himself.
The cost of nasal decolonization: a Kleenex, $15 for a package of swabs and 2 minutes of a pre-op nurse's time. The payoff: fewer MRSA or associated wound infections. A lot fewer.
"Compared to the cost of one infection, I'd say our return on investment was a positive one, as our colon SSI rate decreased significantly," says Maria Sliwinski, RN, BSN, MHHS, CNOR, clinical resource specialist for surgical services at St. Elizabeth Boardman, which trialed and implemented nasal antiseptic decolonization to its SSI bundled interventions a few years ago to address a widespread MRSA problem, knowing that nasal S. aureus is a major risk factor for a surgical site infection.
Among the hospital's total joint and colon resection patients, the MRSA infection rate had been as high as 16.4% in 2013. Yes, nearly 1 of every 6 total joint and colon resection patients contracted a surgical site infection. The hospital fought back with an infection prevention bundle that included:
- a night before/morning of protocol consisting of cleansing with antibacterial soap the night before, CHG bath cloths the night before/morning of surgery, and instructions to don clean pajamas and to sleep in freshly laundered bedding;
- CHG and isopropyl alcohol skin prep in surgery; and
- MRSA swab testing of patients (if positive result, treatment ordered).
The 3-pronged plan looked good on paper, but the MRSA infections persisted among joint and colon resection patients. Turns out, there was a timing problem. The hospital would swab-test for MRSA during pre-admission testing, but wouldn't always have MRSA results at the time of surgery, says Ms. Sliwinski.
The fix was simple: With the advent of povidone iodine and ethanol nasal decolonization products, the hospital decided to decolonize all joint and colon patients on the morning of surgery, as well as wash their skin with a CHG wipe. The one-two punch of nasal and skin decolonization worked. By 2017, the infection rate among joint and colon patients was down to 3.1% throughout St. Elizabeth Boardman and 2 local affiliated hospitals, which also implemented universal decolonization with nasal swabs and CHG wipes as an adjunct to infection control measures on all orthopedic and abdominal bowel patients.
"If we can prevent one infection, it pays to have our bundled process in place," says Ms. Sliwinski. "It's a patient safety initiative that helped to substantially decrease infection rates and ultimately led to great cost savings for our regional facilities."
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)