Simple solutions are almost always best. No one will accuse your facility of providing groundbreaking surgical care if you make sure patients clean their skin before they arrive for surgery, your staff follow proper skin prepping and hand hygiene protocols, and nasal decolonization is part of your pre-op routine. Still, it's always a good idea to brush up on infection prevention's basic protocols and make sure they're being followed in your facility for a very practical reason: They work.
- Home
- The Magazine
- Article
5 Steps to Fewer SSIs
By: Adam Taylor
Published: 11/14/2019
Don't ignore the bacteria-fighting benefits of a back-to-basics approach to infection control.
1. Skin prepping
Instruct patients to use chlorhexidine gluconate (CHG) wipes or bathing solution on the days leading up to surgery, and make sure they understand the solution and the importance of doing so, says Luci Perri, RN, BSN, MSN, CIC, FAPIC, founder and president of Infection Control Results, a North Carolina-based consulting firm.
Patients can be educated on how to use CHG wipes or bathing solution during a pre-op clinic appointment. You can also distribute the wipes or solution in kits that include directives on how and when to apply the CHG and bottles containing the specific amount of solution that should be used during each application. Some facilities even use engagement apps to send patients text message reminders when it's time to apply the CHG.
Ms. Perri says you can't always be certain of how well — or if —patients prep their skin before they arrive for surgery, so she suggests applying CHG in pre-op on and around the intended surgical site to ensure the bacterial count on the area is decreased.
Providing patients with clear wound care directives in discharge instructions is just as important as the efforts you make before surgery to reduce infection risks, notes Ms. Perri, recalling a case where a patient, due to inadequate discharge information, didn't bathe for a week after his procedure.
Also be sure to properly apply skin prepping solutions in the OR. "It's important to follow the manufacturer's instructions," says Ms. Perri. For example, studies suggest it's best to apply a chlorhexidine gluconate-isopropyl solution using a back-and-forth technique as opposed to the circular application techniques suggested by most povidone-iodine prep manufacturers.
2. Nasal decolonization
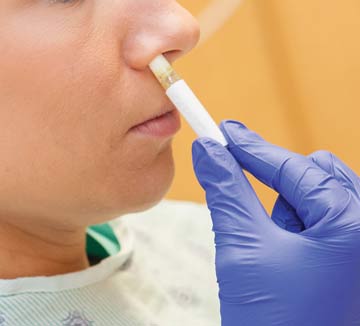
Studies have shown that approximately 80% of surgical site infections are caused by bacteria that originates from the patient's nasal flora, findings that point to the importance of nasal decolonization. You can screen all patients for MRSA in the weeks leading up to surgery to identify and treat carriers with the topical antibiotic mupirocin, but coordinating the screening and the prescribing is labor intensive for providers, adds more clinic appointments for patients and could contribute to the growing issue of antibiotic resistance. Plus, there's no guarantee that carriers who are prescribed mupirocin will comply with the required application regimen.
For those reasons, there's a growing movement to assume all patients are carriers when they arrive at your facility on the day of surgery and treat their nares with povidone-iodine or an alcohol-based nasal sanitizer.
At Temple University Hospital in Philadelphia, Pa., pre-op staff members weren't always treating patients' nares with povidone-iodine simply because nurses had to walk to a different unit to get it, which wasn't always possible. The opportunity to apply povidone-iodine to patients before they went into the OR was therefore sometimes lost. The simple step of storing the prepping agent at the point of use solved the issue, says Mary Mahabee-Betts, MSN, RN, CNOR, the perioperative quality and patient safety nurse manager at Temple.
3. Hand hygiene
Ms. Perri reminds her clients to clean their hands before and after each patient contact, after gloves are removed and after contacting high-touch surfaces such as computer keyboards.
Temple doubled the number of sanitizing gel dispensers throughout the surgical unit to make sure staff members had convenient access to the solution. There are numerous waterless hand rubs available, and each recommends a different application process, "so it's important to follow the instructions for the ones you're using," says Ms. Perri.
4. Instrument care
Surgical instruments should be pre-cleaned at their point of use with a facility-approved product, such as an enzymatic gel. When taking used sets to the instrument reprocessing area, transport them in a securely closed container that's marked with a biohazard label.
To help sterile processing techs who are often under pressure to return sterilized instruments to the ORs as soon as possible, Ms. Perri suggests creating abbreviated cleaning instructions that can be taped onto the wall above decontamination sinks. That's especially helpful for often-used complex instrumentation such as robotic or orthopedic sets.
"Techs have a step-by-step guide right above the sink, and they can read it as they go," says Ms. Perri. "Any instrument reprocessing instructions that require special steps should be posted on the wall."
You should also insist on receiving loaner instrument trays at least 24 hours before the scheduled procedure they'll be used in to give the sterile processing team plenty of time to properly disinfect and sterilize the tools.
5. Limited OR foot traffic
This issue is becoming more important than ever, with lengthier and more complex procedures such as total joints becoming commonplace in outpatient facilities. Temple's cardiac team created a large "Do Not Enter" sign that hangs above the main OR entrance. The hospital also had to educate staff to not enter rooms during procedures to ask the surgical team questions that weren't pertinent to the surgery that was taking place. Temple also continues to enforce a policy that prohibits staff from wearing surgical scrubs outside of the facility and then into the OR.
Tracking progress
Temple's cardiac unit experienced a spike in surgical site infections in the summer of 2016. The creation of the unit's OR Surgical Site Infection Report to monitor SSI prevention protocols led to better adherence to good practices, which led to a gradual decrease in SSIs: 11 from June 2016 to July 2017, 5 in 2017-2018 and 2 in 2018-2019.
The OR Surgical Site Infection Report is a comprehensive electronic reporting tool that lets surgical team members capture and track key aspects of the hospital's SSI bundle, including antimicrobial prophylaxis (timing, selection and duration of therapy); chlorhexidine bathing, both pre- and post-operatively; nasal decolonization; tight glycemic control; and surgical wound care.
Lyndelyn Javier, RN, BSN, RNFA, service line manager of Temple's cardiac, vascular and abdominal organ transplant units, suggests creating a clinical pathway involving a step-by-step guide that doesn't allow patients to move forward along the perioperative pathway until each infection prevention step along the way has been completed.
That wasn't always the case at Temple, where various members of the patient care team documented that infection prevention steps had been completed in various fields within the OR Surgical Site Infection Report — and sometimes even on slip sheets. As a result, the results of the hospital's infection control practices were hard to measure.
That's all changed now that the hospital implemented its electronic reporting system, which captures defined data points for each patient in the same places each time, so completed steps in the SSI-prevention bundle and other key information are now seen in a timely fashion.
"We found out we weren't as good as we thought we were," says Ms. Mahabee-Betts.
Now, they have a clear way of making sure that what's supposed to be getting done really is accomplished as they continue to move toward zero post-op infections. OSM
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)