If you want to roll out a patient warming protocol that requires your facility to invest time, resources money — and, of course, a change to the status quo — you need to give leadership a compelling reason why the move is a worthwhile investment. We knew that active patient warming helps to prevent unplanned perioperative hypothermia, but our hospital didn't have a standardized method to warm patients, so we gradually launched a successful prewarming protocol across our entire orthopedic service line, and what we learned during the process could convince you to make changes to your own patient-warming protocols.
- Home
- The Magazine
- Article
Warming Works Wonders
By: Kathy Abbott
Published: 2/3/2021
We trialed prewarming on a small group of patients, and now interest is heating up among multiple specialties.
Starting small
Your first order of business is to create a warming protocol that's effective, repeatable and right for your facility. You don't have to reinvent the wheel; there are plenty of resources available to guide you, including evidence-backed guidelines from organizations such as AORN. Obviously, the protocol will vary from facility to facility, and there are a number of different warming methods to choose from (forced-air warming, conductive fabric devices, circulating water devices), but the most important component is choosing a process that employs active warming, which, as the name suggests, warms patients with an external source of heat, as opposed to passive warming tactics, which only prevent insulation against heat loss — warm blankets, for example.
I also recommend starting small. Procedural changes are a tough sell, especially when those changes involve multiple staff levels (nurses, surgeons, techs and anesthesiologists). After some open discussions with our surgeons and anesthesiologists about our options, we decided to prewarm neuromuscular (NM) spinal fusion patients with warming gowns. While we eventually made changes to all our orthopedic procedures, we started with this small subset of patients, a group that is significantly exposed during surgery. We'd always had trouble maintaining normothermia (core body temperature of 36°C) in them, and we needed to protect this vulnerable group from the many potential adverse reactions of hypothermia — infection, poor wound healing, increased blood loss (and the potential need for a transfusion), decreased renal function and prolonged hospitalization.
For our initial trial, the vendor provided one box of 20 gowns and three warming units free of charge. After the trial, it cost us $8.23 per gown to prewarm patients, a cost our hospital's leadership saw as a reasonable investment in safety.
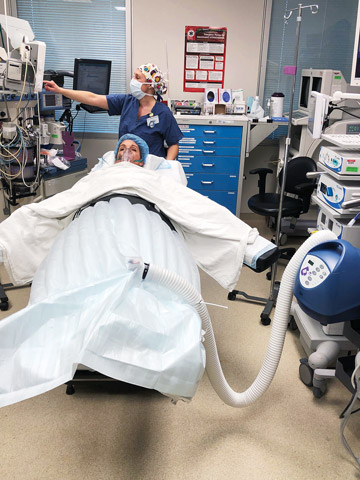
When you educate staff on new patient warming protocols, break down the process into a series of easy-to-follow steps:
- Have the pre-op nurse place a body-warming blanket on the stretcher.
- Place the patient on the stretcher.
- Put the warming gown on the patient.
- Attach the warming unit to the gown and have the pre-op nurse set the temperature to "high."
- Detach the warming unit when the patient is transported to the OR, and keep the detached unit in pre-op.
- Have the OR nurse attach and turn on the patient's underbody-warming blanket as soon as they arrive in the OR. (This step ensures active warming continues during the induction, intubation, IV start, central line placement, urinary catheter insertion and placement of pressure site padding).
- Lower the setting of the body-warming blanket during the procedure.
These are the basic steps to our protocol, but we make constant tweaks and variations. For instance, even though our pre-op nurse will always set the warming gowns temperature to "high," patients often adjust that setting based on personal comfort. Patient temperatures are checked once pre-operatively via a temporal scan (across the forehead to behind the ear), and intraoperatively on a continuous basis after induction via an esophageal temperature probe.
On the same page
Every protocol change is ultimately a communication issue, and effective communication is rarely a simple process. What gets through to one group is often ineffective or confusing for another. Whenever an initiative involves a multidisciplinary team, you often need to deliver the message in multiple ways (face to face, email, real-time education and follow-up training when an issue arises).
Every policy change is ultimately a communication issue, and effective communication is rarely a simple process.
We did that, but no matter how comprehensive our communication was, issues still cropped up. For instance, new pre-op RNs often weren't notified of the protocol. Or they were, but didn't retain the information after orientation. Our pre-op also has several protocols for other interventions (SCD application, IV starts, etc). That's why we developed a quick and easy algorithm to reference whenever there was a question as to whether a patient would be actively warmed before surgery.

The algorithm uses medical history (for example, history of neuromuscular conditions such as cerebral palsy or spastic quadriplegia), patient BMI and length of surgery (less than or more than two hours) to help providers determine if the patient should be prewarmed. For instance, after the initial medical history question, patients are grouped according to BMI. Our team actively warms patients with BMIs less than 25 undergoing surgery lasting longer than two hours. We chose the less-than-25-BMI threshold to ensure we don't actively warm overweight or obese patients, who are at less risk of becoming hypothermic during surgery. We chose two hours as our length-of-surgery benchmark because most ortho procedures that are less than two hours don't result in significant blood loss, which has been linked to unplanned perioperative hypothermia.
The algorithm is a simple visual guide to direct providers who may not be versed in our warming protocols. While the completed algorithm is a very simple tool, its creation was a process — with several changes in format before we settled on the version and metrics we're using today. If you're planning on creating an algorithm at your facility, you need to function as a team and solicit and implement staff feedback.
Warming trend
I was optimistic about the prewarming trial, but the results exceeded even my own expectations. Each of the initial six participating surgeons agreed to implement the warming protocols on a permanent basis. Plus, anesthesiologists were extremely vocal about how the active prewarming made an immediate difference in their abilities to maintain normothermia among NM patients. Not only have we added the protocol to all ortho patients who fit the algorithm's criteria and our NUSS patients in general surgery, several leaders of neurology, ENT, urology, ophthalmology and plastics service lines are interested in adding the algorithm to their respective protocols. Our efforts show you can make big changes and get major results — as long as you're willing to put in the work and take the time to get all staff members and providers involved to buy into the change. OSM
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)