Ophthalmology is a physically demanding specialty. Surgeons spend good portions of their day looking through the eyepieces of surgical microscopes, leaning forward in unnatural positions while performing delicate microsurgery that requires minute hand movements. They adjust their chairs and reposition the patient, but are often forced to endure ergonomically unfavorable positions that put stress on their back, neck, arms and even their eyes.
I’ve been practicing for 20 years and perform between 75 and 100 cataract surgeries a week. Although each procedure takes me only about five minutes to complete, the cumulative effects of ergonomic stress can take their toll. The repetitive nature of working in ophthalmology has been shown to cause long-lasting degenerative and physiologic changes to the vertebrae that lead to scoliosis, bulging discs and arthritis of the neck and spine in the lumbar thoracic and cervical regions. Many surgeons have suffered short- or long-term disabilities throughout their careers.
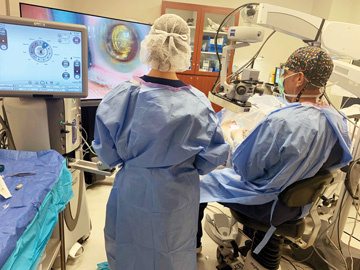
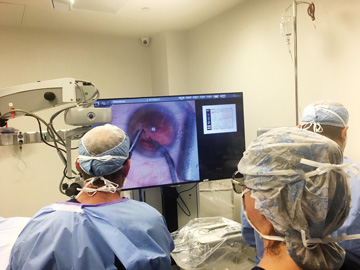
These concerns led me to adopt heads-up 3D visualization, which frees me from sitting behind a surgical microscope for hours at a time. I’ve had lower back issues for most of my adult life and underwent a microdiscectomy due to sports-related injuries. It’s important for me to be in a comfortable position when I operate to protect my back and guard against developing other chronic issues. I’ve experienced significantly less neck and back pain since performing heads-up cataract surgery, but that’s only one of the reasons I rely on the technology at my practice.
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)