If you're running a successful outpatient total joint program and want to increase case volumes, the future is bright. Last year, CMS began paying for total knees performed in ASCs and this year gave surgery centers the green light to take on total hips. In addition to an influx of Medicare cases, increasing numbers of patients with private insurance are buying into the benefits of having their joints replaced at freestanding facilities.
In the coming years, I believe the only joint replacements done on an inpatient basis will be complex revisions, repairs of periprosthetic fractures and procedures performed on patients without at-home support who require hospitalization and a stay at a rehab facility after surgery.
There's no need to wait for these factors to positively impact your facility, however. By focusing on preoperative medical optimization of patients, constantly fine-tuning your clinical protocols and remaining focused on the best practices of same-day surgery, you can take your total joints program to the next level right now.
The surgery center my partners and I founded in 2013 is about to surpass 12,000 joint replacements performed. Our team does about six cases each day — nearly an even split between partial knees, total knees and total hips — in each of the center's two operating rooms. We've been able to approach that major milestone by constantly focusing on these pillars of proven success.
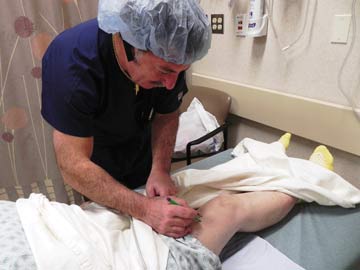
- Patient selection. With Medicare now paying for hip and knee replacements performed in surgery centers, consider expanding the pool of potential surgical candidates to include older and heavier patients. I don't have any cutoffs when it comes to age or BMI, but all of my patients must be medically optimized before their procedures. We make sure elevated hemoglobin A1C is corrected and any hint of a cardiac issue is assessed and addressed. The medications patients are on are evaluated. A family practitioner or internist must confirm a patient's heart and lungs can handle the stress of surgery. The physicians we work with specialize in preoperative assessments and know they have full authority to tell me whether a patient should have their procedure done in our surgery center or a full-service hospital.
.svg?sfvrsn=be606e78_3)

.svg?sfvrsn=56b2f850_5)