Same-day shoulder replacements are very much in their infancy, but the migration from inpatient hospitals to ambulatory ORs is moving fast. In fact, the rate at which shoulder replacements are increasing is higher than total knees and hips. This industry-wide relocation will only speed up — CMS is whittling its inpatient-only list and shoulder arthroplasty is on tap for removal. At Penn Medicine, where I practice, about 300 to 400 total shoulders are performed each year. Many are still done inpatient, but it's only a matter of time before these procedures make the move to outpatient facilities. Focusing on these essential elements of shoulder replacement success will position your facility to capture case volumes that are certain to increase in the coming years.
- Pre-op assessments. You need a competent clinical team that confers with surgeons and anesthesia providers to identify appropriate candidates for outpatient shoulder replacements. The best candidates for outpatient shoulders have healthy BMIs and no comorbidities such as congestive heart failure, COPD, immunodeficiencies or severe shoulder deformities. I've operated on patients in their teens and some in their nineties, but the majority of patients are arthritis sufferers in their sixties, seventies and eighties. As a new endeavor, you should err on the side of caution until your program is up and running and your team gains experience in performing the procedures and managing patient care.
- Anesthesia pros. Having a good anesthesia team that is skilled at administering regional blocks and willing to communicate with patients about what to expect before and after blocks are placed is paramount. Nerve block recipients will experience numbness in their arm, and perhaps even lack the ability to use their arm for a day or so after their surgery. This could cause undo anxiety if they're not told to expect the lack of sensation in advance, as they'll think it's abnormal and a potentially serious complication. You need an anesthesia group that not only answers calls from concerned patients, but that checks in on the patients proactively after procedures to assess their condition and answer questions they have.
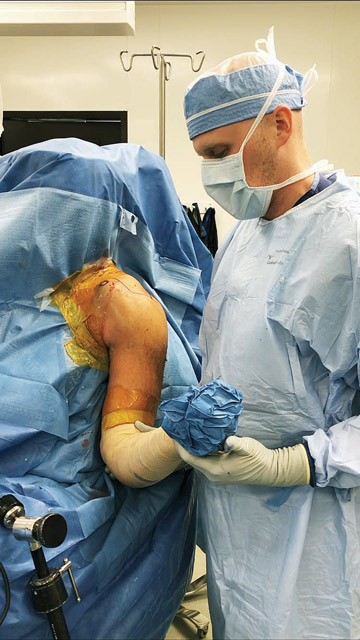
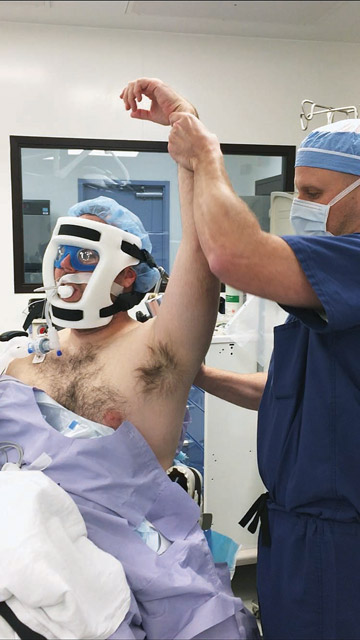
- In the OR. Surgical tables should recline so the patient can be placed in the beach chair position, which is the only option for shoulder replacement surgery because it allows surgeons to see all areas of the joint in an anatomically correct way.
Patients should be reclined at approximately 45 degrees to offload pressure on the sciatic nerve and specialized attachments are needed to stabilize the head, including a foam mask that supports the patient during the entirely of the procedure. Attachment are also available that allow surgeons to position the arm in a way that provides optimal access to the surgical site.
The 6cm to 8cm incision is made with dissection through the deltopectoral total interval, down to the fascia and under the conjoint tendon. The subscapularis muscle is approached and removed from the humerus with either a peel or osteotomy. The shoulder is then dislocated, and the replacement performed. Implants are typically placed based on pre-op planning and surgeon experience. Cases range from one to two-and-a-half hours, depending on the patient and the severity of their arthritis.
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)